Our Blog
Discover expert tips, health information, and clinic news to support your wellness journey.
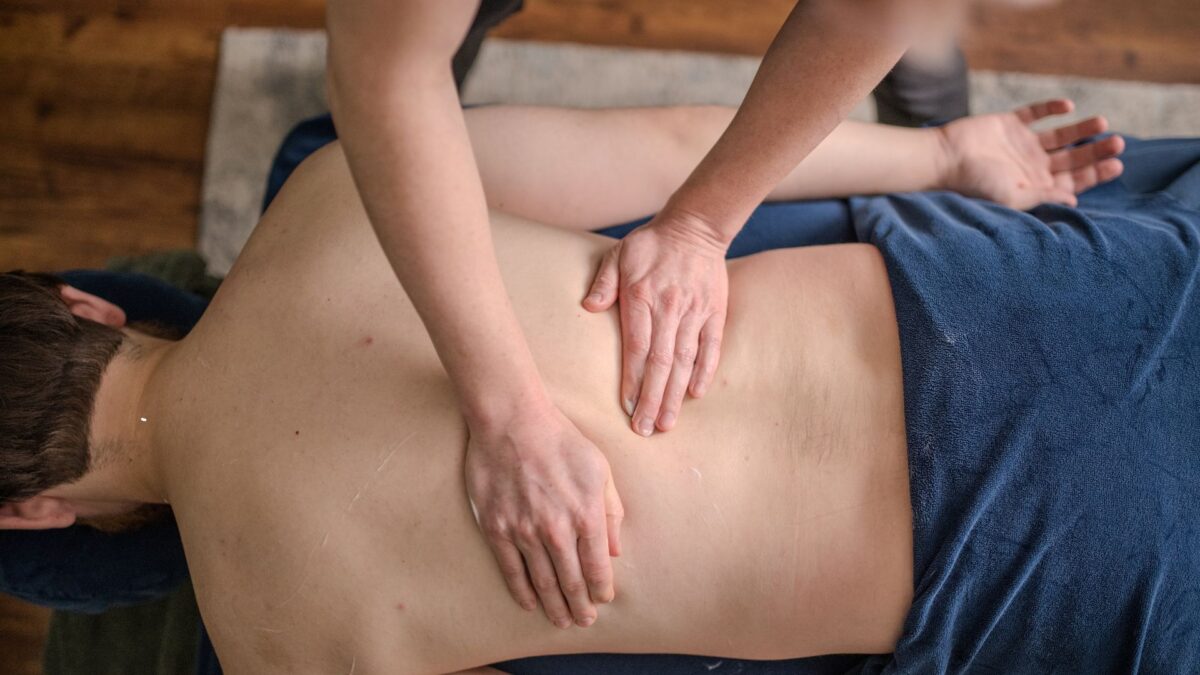
Deep Tissue vs. Relaxation Massage: How to Choose the Right Treatment
The Massage You Need Isn’t Always the One You Think If you’ve ever stared at a massage menu trying to figure out what you actually …
5 Signs Your Body Is Asking for Therapeutic Care
You Don’t Need To Be In Crisis To Deserve Care Many of our clients at All Deep Massage & Wellness tell us the same thing …
Cold Weather, Tight Muscles: Understanding and Treating Winter-Specific Pain
You’re Not Imagining It: Winter Really Does Make Pain Worse If you’ve noticed your body hurts more in winter, you’re not imagining it. That shoulder …
Sciatica vs. Piriformis Syndrome: How to Tell the Difference
Shooting Leg Pain? It Might Not Be What You Think That shooting pain down your leg – is it sciatica? Piriformis syndrome? Something else entirely? …
Why Your Chronic Pain Keeps Coming Back (And How to Finally Break the Cycle)
Understanding Your Body’s Hidden Pain Patterns You’ve tried everything. Physiotherapy, chiropractic care, massage, stretching, strengthening exercises, anti-inflammatories, heat, ice – maybe even surgery. You feel …
What Are Trigger Points? Understanding Your Body’s Pain Signals
Why Those “Knots” Hurt – And How to Release Them Ever press on a spot in your shoulder and feel pain shoot down your arm? …
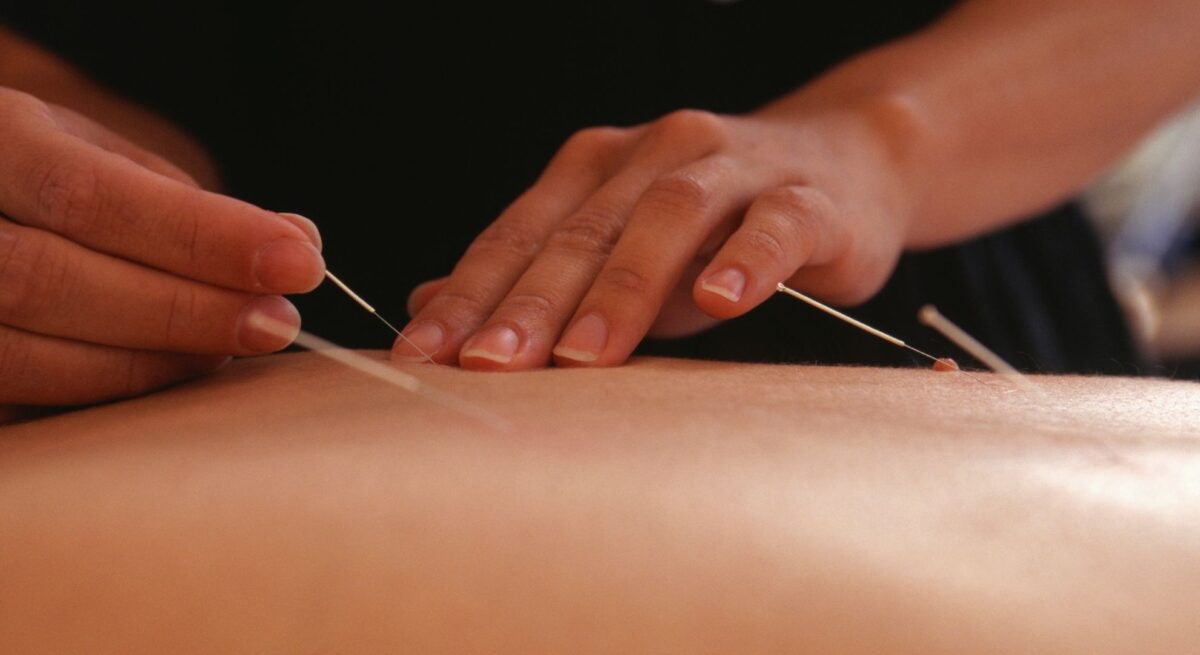
Acupuncture Myths Busted: Separating Fact from Fear
What Research Really Says About Acupuncture Let’s clear the air about one of the world’s oldest healing arts. Acupuncture has been helping people heal for …
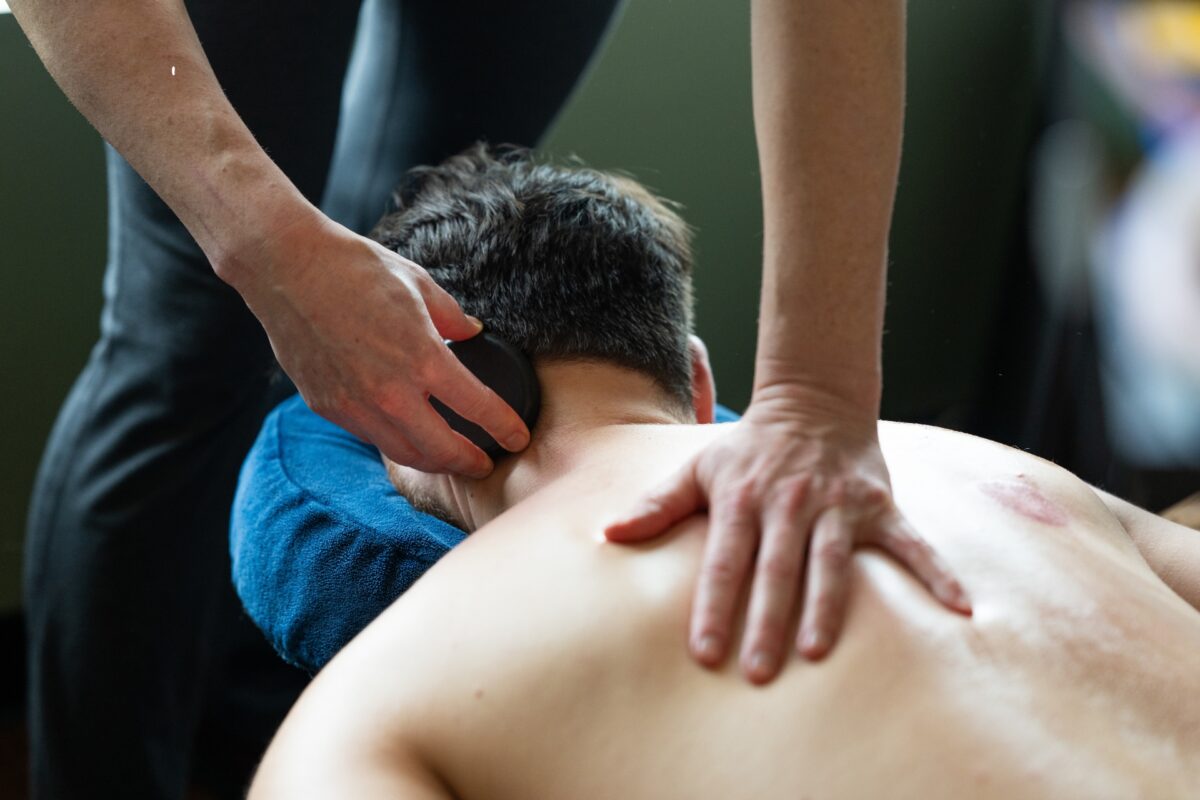
4 Compelling Reasons to Choose a Hot Stone Massage
Discover the Therapeutic Power of Heat and Touch Combined There’s something almost magical about the combination of skilled therapeutic touch and the penetrating warmth of …
Lymphatic Massage in Sherwood Park: Boosting Your Body’s Natural Detoxification
Discover the power of lymphatic massage at All Deep Massage & Wellness in Sherwood Park. Learn how this gentle technique boosts natural detoxification, enhances immunity, and promotes overall well-being.
The Transformative Power of a Head Massage
In today’s fast-paced, high-stress world, it’s more important than ever to prioritize self-care and relaxation. At All Deep Massage & Wellness in Sherwood Park, we believe that holistic healing practices, such as head massage, can play a crucial role in promoting overall well-being.