5 Sports Injuries That Massage and Acupuncture Can Help: Effective Relief Techniques
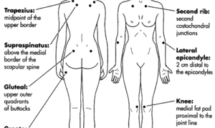
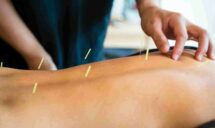
Sports Injuries That Can Benefit from Massage and Acupuncture Therapy The world of competitive sports is thrilling but can also be demanding on the body, often leading to injuries that impede performance and cause pain. Among the various treatment modalities, massage and acupuncture have emerged as powerful tools for addressing sports-related injuries. These therapies are […]
Mar 27, 2024